Introduction
Direct visualization of the biliary ductal system is quickly gaining importance among gastroenterologists. Since the inception of cholangioscopy in the 1970s, the technology has progressed, allowing for ease of use, better visualization, and a growing number of indications. Conventional endoscopic retrograde cholangiopancreatography (ERCP) is successful for removal of bile duct stones (with success rates over 90%);1 however, its use in the evaluation of potential biliary neoplasia has been somewhat disappointing. The diagnostic yield of ERCP-guided biliary brushings can range from 30% to 40%.2-4 An alternative to ERCP-guided biliary brushings for biliary strictures is endoscopic ultrasound (EUS)-directed fine needle aspiration (FNA), but the reported sensitivity remains poor, ranging from 43% to 77% with negative predictive values of less than 30%.5-7 These results leave much to be desired for diagnostic yield.
The newest method of evaluating pancreaticobiliary pathology is with direct visualization using cholangioscopy. The advantages of this modality include the ability to obtain direct visualization as well as targeted biopsies of suspicious lesions. The first fiberoptic cholangioscope was introduced in 1965 and the first use of peroral cholangioscopy was reported in in the mid 1970s.8,9 Early models were limited by their delicacy, relative immmobility, lack of dedicated irrigation channel, and need for two endoscopists using a “mother baby” design. Fiberoptic single-operator cholangiopancreatoscopy (FSOCP) was first introduced in 2006 by Boston Scientific (Marlborough, MA).10 It was designed to address the previously stated shortcomings of the first-generation cholangioscopy devices. Since its introduction, it has gained worldwide popularity in the diagnosis and management of pancreaticobiliary pathology and complex biliary stones.The initial model employed a reusable fiber optic optical probe, a disposable cholangioscope access and delivery catheter, and disposable small-caliber biopsy forceps. The components can be introduced through a duodenoscope that has a minimum working channel diameter of 3.4 mm. The original FSOCP catheter is attached to the duodenoscope by a silastic belt just below the operating channel, allowing for single operator use. The access and delivery catheter has an outer diameter of 10 F and three separate ports: an optical port, two dedicated 0.6-mm irrigation channels, and a 1.2-mm accessory channel that accepts various accessories including the small-caliber biopsy forceps, electrohydraulic lithotripsy (EHL) fibers, or a holmium laser probe. The catheter has fourway tip deflection. The fiberoptic probe does have limitations, including its limited field of view, fragility of the fiber, and need for adjustment of the lens focus. Because of these limitations, a digital single-operator cholangioscope (DSOCP) was developed and introduced in 2014 (Boston Scientific, Marlborough, MA). In the DSOCP system, the light is generated by two independent light-emitting diodes and a complementary metal-oxide semiconductor digital camera chip. Improvements included a wider 120-degree field of view, dedicated irrigation and aspiration channels/connections, suction channel, and redesigned accessory channel. The cholangioscope is entirely disposable. The processor receives video signals from the catheter, processes the signals and outputs video images to an attached monitor. The newer digital-based platform has shown promising results, including higher diagnostic yield and shorter ERCP completion time when compared with similarly performed procedures using the fiberoptic-based platform.11Clinical indications
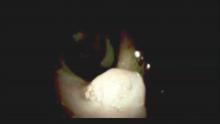
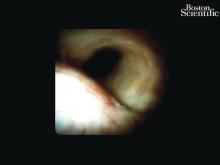
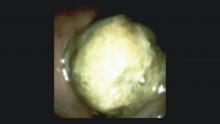
Direct visualization and biopsy of indeterminate biliary strictures has resulted in greatly improved diagnostic accuracy and collection of adequate tissue (Figures. 1,2). In a recent systematic review, the pooled sensitivity and specificity of cholangioscopy-guided biopsies in the diagnosis of malignant biliary strictures was 61% (95% confidence interval, 55%-65%) and 98% (95% CI, 96%-99%), respectively. Direct comparison of small-caliber direct biopsies with standard brushings and biopsies showed small-caliber direct biopsies having a sensitivity of 76.5% versus 5.8% and 29% with standard brushes and biopsies, respectively.12 The pooled sensitivity and specificity of six studies using cholangioscopy with targeted biopsies in the diagnosis of cholangiocarcinoma was 66.2% and 97.0%, respectively.12 Studies have shown that small-caliber forceps obtains tissue adequate for pathologic evaluation in 82%-97% of biopsy samples retrieved.13-17 Three prospective trials have evaluated the diagnostic accuracy of small-caliber forceps for indeterminate biliary lesions. The accuracy ranged from 72% to 85% with a sensitivity of 49%-82%, specificity of 82%-100%, positive predictive value of 100%, and negative predictive value of 69%-100%.15-17 The improved diagnostic accuracy of cholangioscopy for indeterminate biliary strictures stems from its direct visualization ability. Traditional sampling techniques (cytology brushings and fluoroscopically guided biopsies) are plagued by low sensitivity and negative predictive value caused by a relatively high false-positive rate.DSOCP appears to have improved accuracy over fiberoptic equipment. In a recent multicenter observational study in patients undergoing digital cholangioscopy, the guided biopsies resulted in adequate tissue for histologic evaluation in 98% of patients. In addition, the sensitivity and specificity of digital cholangioscope-guided biopsies for diagnosis of malignancy was 85% and 100%, respectively.11
Other less common diagnostic indications for DSOCP include evaluation of cystic lesions of the biliary tract, verifying clearance of bile duct stones, bile duct ischemia evaluation after liver transplantation, hemobilia evaluation, removal of a bile duct foreign body, and evaluation of bile duct involvement in the presence of an ampullary adenoma.3,14,15,20,26,27