Aneurysmal bone cysts (ABC) are expansile, hemorrhagic, non-neoplastic lesions that can be locally destructive1 and that can arise either de novo or secondary to another benign or malignant lesion.2 Although primary and secondary ABCs typically are benign, there are cases of malignant degeneration of primary ABCs, though the transformation arises almost exclusively in the context of prior radiation exposure.3-5 Malignant change without history of irradiation is rare; only 6 such cases have been reported.5-10 In 4 of these cases, the transformation was to osteosarcoma.5,8-10
Here we report on an ABC that degenerated into a fibroblastic osteosarcoma—the fifth such case in the medical literature. In addition to reviewing the earlier cases, we describe the radiologic and histologic underpinnings of this diagnosis and the insight that they provide into the pathogenesis of this rare process. Although the prevailing view is that ABCs are benign, it is important to know these lesions have the potential to undergo malignant transformation, even in the absence of prior radiation exposure. The patient provided written informed consent for print and electronic publication of this case report.
Case Report
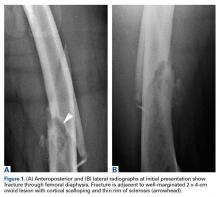
A healthy and previously asymptomatic 37-year-old man presented with thigh pain after a minor fall onto a couch. Radiographs showed a diaphyseal femoral pathologic fracture adjacent to a small but benign-appearing cystic lesion (Figures 1A, 1B).
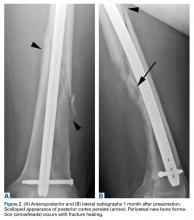
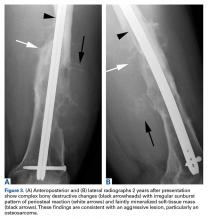
At another institution, the patient underwent incisional biopsy through a lateral trans-vastus approach before antegrade intramedullary interlocked rod fixation. The histologic specimen was reported by the referring pathologist as being consistent with a unicameral bone cyst with hemorrhage. The patient returned for only 1 follow-up visit, 1 month after fracture fixation, and radiographic findings were similar—a benign-appearing cystic bone lesion adjacent to a healing fracture (Figures 2A, 2B). He had mild persistent thigh swelling, which did not interfere with daily activities, and he did not seek further medical attention.Two years later, the patient had a bicycle accident and, after 2 weeks of significantly increased thigh swelling, presented to the emergency department at the referring institution. Radiographs showed a lytic lesion in the femoral diaphysis that was highly suspicious for malignancy (Figures 3A, 3B).
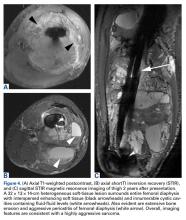
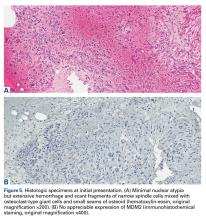
The patient was transferred to our institution. Clinical examination revealed an extensive firm mass in the mid to distal thigh. Magnetic resonance imaging (MRI) showed an aggressive, multilobulated mass surrounding the mid to distal femoral diaphysis (Figures 4A-4C).The initial biopsy specimens were evaluated at our institution and interpreted as being consistent with an ABC, with negative immunohistochemical staining for MDM2 (Figures 5A, 5B).
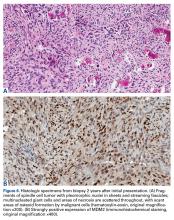
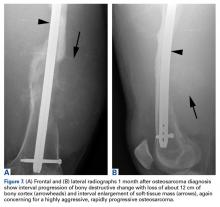
A repeat incisional biopsy of the thigh soft-tissue mass was performed, and its results showed a high-grade osteosarcoma that was markedly positive for MDM2 (Figures 6A, 6B). The constellation of initial imaging findings (benign-appearing cystic lesion) and histologic appearance without MDM2 staining plus subsequent imaging findings (aggressive, multilobulated mass) with histology positive for MDM2 was considered evidence of sarcomatous degeneration of a primary ABC. Radiographs obtained 2 weeks after the osteosarcoma diagnosis showed worsening bone erosion (Figures 7A, 7B).The patient underwent a 3-month course of neoadjuvant chemotherapy with cisplatin and doxorubicin. Interval-staging contrast-enhanced chest, abdomen, and pelvis computed tomography (CT) showed no evidence of metastatic disease. Preoperative MRI showed a significantly larger heterogeneous mass, now with neurovascular involvement, which precluded limb salvage.
The massive size and proximal extent of the tumor required hip disarticulation for local control. Areas contaminated by the prior surgery, including the entry site of the antegrade rod and surrounding gluteal musculature, were resected widely, en bloc, with the amputation specimen. The surgical margins were widely free of tumor. Necrosis in response to chemotherapy was <1%. Histologic analysis revealed a heterogeneous 35-cm tumor with areas similar to those on the initial biopsy specimen (2 years earlier) intermixed with areas consistent with high-grade osteosarcoma (Figures 8A–8D). Adjuvant salvage chemotherapy was continued, and the patient had no evidence of tumor recurrence or metastatic disease more than 2 years after surgery.Discussion
Aneurysmal bone cysts are expansile, hemorrhagic, locally destructive lesions that generally develop within the first 3 decades of life. Ever since they were first described by Jaffe and Lichtenstein11 in 1942, the most widely accepted theory of their pathogenesis has been that they begin as a benign reactive vascular process.12 However, more recent molecular studies by Oliveira and colleagues13 and Panoutsakopoulos and colleagues14 have demonstrated a clonal neoplastic basis for primary ABCs related to cytogenetic upregulation of oncogenes USP6 and CDH11 after translocation of 17p13 and 16q22.