Case Reports
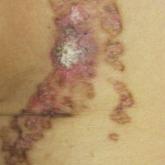
Linear Porokeratosis Associated With Multiple Squamous Cell Carcinomas
Linear porokeratosis is a rare subtype of porokeratosis with a higher rate of malignant transformation than other subtypes of porokeratosis....
Dr. Nguyen is from the Creighton University School of Medicine, Phoenix Regional Campus, Arizona. Drs. Glembocki and Patel are from Southwest Skin Specialists, Phoenix.
The authors report no conflict of interest.
Correspondence: Austin Huy Nguyen, MD, MS, Creighton University School of Medicine, Phoenix Regional Campus, 350 W Thomas Rd, Phoenix, AZ 85015 (AustinNguyen@creighton.edu).

Presentation
A systematic review of published reports determined that 79% of MCAH cases occur in females, with an average age of onset of 50.1 years.2 However, MCAH likely is underreported due to the overall lack of knowledge regarding this condition by physicians and pathologists. The hands and face are the most commonly affected areas, though other sites of involvement have been reported, including the lower extremities,3,4 oral mucosa and upper lip,5,6 and trunk,7,8 as well as generalized distribution.9-12 Additionally, 1 case presented as a single plaque on the trunk rather than having papular or nodular morphology.8 Multinucleate cell angiohistiocytoma lesions generally are asymptomatic, though pruritus may be present.13 The condition is regarded as benign, though a minority of cases have exhibited spontaneous resolution.14-16
Histopathology
Multinucleate cell angiohistiocytoma histology demonstrates full-thickness dermal microvessel proliferation and fibrosis with characteristic multinucleate giant cells.2,3 Vascular endothelial cells stained positive for CD68 in 60% of cases2 as well as the normal endothelial markers (ie, factor VIII, CD31, CD34). The multinucleate giant cells exhibit immunoreactivity for macrophage/histiocytic markers factor XIIIa and CD68.
Etiology
The pathogenesis of MCAH is not yet fully understood, but it is considered to be a benign vascular or fibrohistiocytic neoplasm.17 Calderaro et al18 described a series of 8 patients who developed MCAH either within a cutaneous neoplastic process or in conjunction with various cutaneous reactive conditions, including hidradenitis suppurativa and chronic radiation dermatitis, as well as overlying a bone prosthesis placed due to degenerative arthritis. These cases suggest that MCAH, or possibly a subset of the disease, is a reactive process. Suggested inciting events include cancer with stromal inflammatory reaction, chronic inflammation (as seen in hidradenitis suppurativa), chronic radiation dermatitis, scarring, and vascular injury.18 Retrospective immunohistochemical evaluation of a series of MCAH cases demonstrated intralesional spindle cells to strongly express estrogen receptor alpha and factor XIIIa. Additionally, these cells sparsely expressed progesterone receptor and demonstrated no vascular endothelial growth factor immunoreactivity.19 This immunohistochemical profile supports MCAH as a distinct entity from dermatofibromas. These findings also suggest a role of hormone signaling, namely estrogen receptor alpha, in MCAH tumor biology and may offer an explanation for the predilection of MCAH in females. Furthermore, estrogen receptor positivity offers a possible mechanism for the highly vascular nature of the lesions, considering the angiogenic properties of estrogen signaling.20 In a systematic review of 142 published cases of MCAH, CD68 positivity on multinucleate cells in MCAH lesions suggested a fibrohistiocytic origin.2 However, a number of these cases exhibited CD34 positivity, thus a macrophage origin may not be excluded.
Differential Diagnosis
The differential diagnosis for MCAH includes Kaposi sarcoma clinically and dermatofibroma and fibrous papules histologically. Sass et al21 determined the in vitro behavior of cultured MCAH cells to contrast markedly with Kaposi sarcoma–derived cells. Although Kaposi sarcoma–derived cells exhibited invasive behavior, cells isolated from MCAH lesions were less elongated and were unable to traverse basement membranes.
Treatment
Surgical excision or cryotherapy appear to be definitive treatments of MCAH; however, a number of cases have reported light and laser modalities as successful alternatives to excision. One case of MCAH affecting the face was treated with pulsed dye laser monotherapy.22 This modality allowed selective coagulation of the vascular structures in MCAH. At 8-month follow-up, the initial lesion was noted to be completely cleared, though similar lesions had recently appeared elsewhere on the face.22 Another case of MCAH affecting the leg was treated with pulsed dye laser and both topical and intralesional corticosteroid combination therapy. In this case, the lesion failed to respond to treatment, which may suggest that facial localization could influence response in pulsed dye laser treatment.3
Intense pulsed light also has been reported as a definitive treatment in 2 cases.2,13 Slight erythema and transient pruritus have been reported immediately following treatment. In this case, complete resolution with only residual hyperpigmentation was reported at 2-month follow-up, with no recurrence during 12 months of follow-up.13
Argon laser therapy has been used in 2 cases. After a single session, lesions were no longer palpable, with no scarring noted at 8 weeks follow-up.23 Lastly, 2 cases of MCAH have been successfully treated with the CO2 laser, with no relapse noted at 2.5- or 5-month follow-up, respectively.24
Multinucleate cell angiohistiocytoma is a rare and likely underdiagnosed dermatologic condition that is believed to be a reactive process. Characteristic histology of MCAH demonstrates microvascular proliferations of the dermis with multinucleate giant cells amidst a fibrous background. Although surgical excision is curative, there are reports in which laser and light therapies were used to effectively treat MCAH.

Linear porokeratosis is a rare subtype of porokeratosis with a higher rate of malignant transformation than other subtypes of porokeratosis....
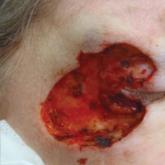
To the Editor: Primary mucinous carcinoma (PMC) is an exceedingly rare adnexal tumor with an incidence of 0.07 cases per million individuals.1,2...
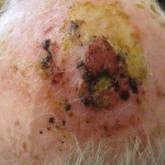
We describe a painful atypical fibroxanthoma (AFX) arising in a setting of erosive pustular dermatosis of the scalp. Complete excision was...
